Table Of Contents
-
Key Highlights
- Understanding Glucometer Test Strips and Their Lifespan
- Factors That Affect When to Replace Your Test Strips
- Proper Storage and Handling to Extend Test Strip Life
- Continuous Glucose Monitors vs. Traditional Test Strips: Replacement Schedules
- Signs Your Glucometer Test Strips Need Replacement
-
Frequently Asked Questions
- Taking Control of Your Glucose Monitoring Accuracy
-
References and Sources
If you’re managing diabetes, you know that accurate blood glucose readings aren’t just numbers on a screen—they’re the foundation of your daily treatment decisions. But here’s something many people don’t realize: the test strips you’re using might be giving you false readings without you even knowing it. The question isn’t just “how often should you replace glucometer test strips,” but understanding the critical factors that determine when these tiny diagnostic tools lose their accuracy.
Whether you’ve just been diagnosed or you’ve been testing your blood sugar for years, understanding proper test strip replacement can make the difference between confident diabetes management and potentially dangerous misinformation. According to the FDA, improper test strip usage and storage accounts for a significant portion of inaccurate blood glucose readings that lead to incorrect treatment decisions.
Key Highlights
- Glucometer test strips are designed for single-use only and must be discarded immediately after each blood glucose test
- Once opened, test strip vials typically remain accurate for 3-6 months when stored properly in their original container with the cap tightly closed
- Using expired glucose test strips can lead to significantly inaccurate readings, risking dangerous treatment decisions
- Environmental factors like humidity, temperature extremes, and direct sunlight can degrade test strips faster than the printed expiration date suggests
- Lot-to-lot variability in manufacturing means test strips from different batches can show accuracy differences of up to 13%, even from the same brand
- Continuous glucose monitor sensors have completely different replacement schedules—typically every 7-14 days for disposable sensors or up to 180 days for implantable systems
- Regular quality control checks using control solutions help verify that both your meter and test strips are providing accurate readings
Understanding Glucometer Test Strips and Their Lifespan
Think of glucose test strips as sophisticated chemical laboratories compressed into a tiny piece of plastic. Each strip contains multiple layers of enzymes and chemicals that react specifically with the glucose in your blood. When you apply blood to the strip, these enzymes trigger an electrochemical reaction that your meter measures and converts into a blood sugar reading.
But here’s what makes these strips so sensitive: those same enzymes that react to glucose also react to moisture, oxygen, heat, and light. From the moment a test strip is manufactured, it begins a slow degradation process. Research published in the Journal of Diabetes Science and Technology explains that proper handling and storage are just as critical as the test strips themselves for accurate blood glucose monitoring.
The Single-Use Nature of Test Strips
Unlike some medical supplies that can be cleaned and reused, glucose test strips are strictly single-use devices. Once you’ve applied blood to a strip, the chemical reaction is complete and irreversible. Attempting to reuse a test strip—even if it looks clean—will give you completely unreliable results. The FDA explicitly warns against buying or using pre-owned test strips for this exact reason.
Shelf Life: Unopened vs. Opened Vials
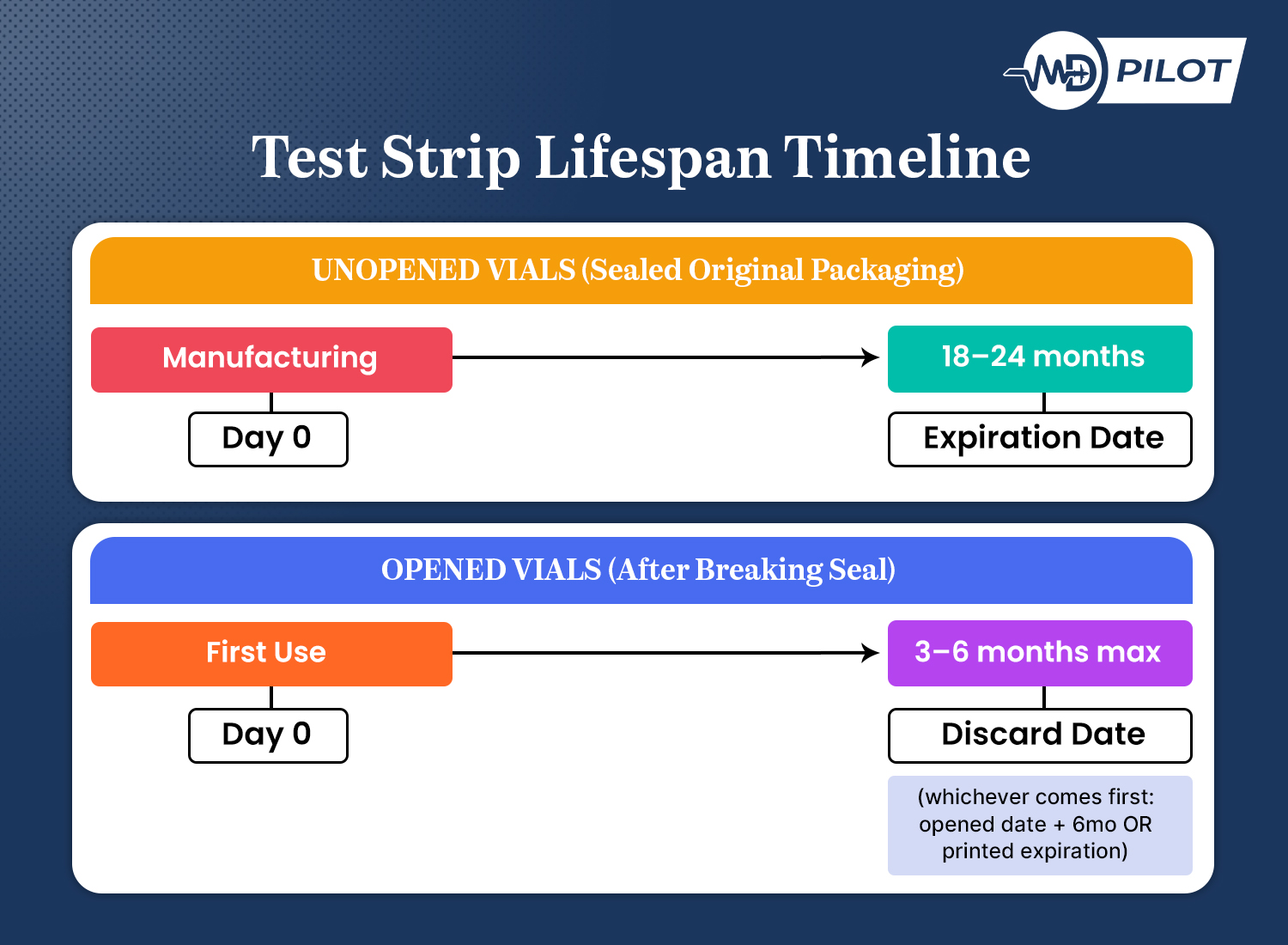
Understanding the two different timelines for test strip viability is crucial. Unopened test strip vials sealed in their original packaging can typically last 18-24 months from the manufacturing date when stored in cool, dry conditions. However, the moment you break that seal and expose the strips to air, you start a much shorter countdown.
Most manufacturers recommend using opened test strips within 3-6 months, regardless of the printed expiration date. This isn’t just a suggestion—it’s based on careful testing of how quickly the strips degrade once exposed to environmental factors. Some brands include a “discard by” date space on the vial label where you should write the date you opened it.
Factors That Affect When to Replace Your Test Strips
Several environmental and handling factors can significantly accelerate test strip degradation, potentially causing you to replace them well before their printed expiration date. Understanding these factors helps you recognize when your strips might be compromised.
Storage Conditions: The Silent Accuracy Killer
Temperature and humidity are the two biggest enemies of test strip accuracy. A comprehensive review on blood glucose testing limitations found that test strip accuracy can decline significantly when exposed to temperatures above 86°F (30°C) or humidity levels above 80% for just one week.
| Storage Factor | ✓ Proper Storage | ✗ Improper Storage | Impact on Accuracy |
|---|---|---|---|
| Temperature | 68-77°F (20-25°C) Stable room temp | Above 86°F or below 40°F car glove compartment | Enzyme degradation accelerates; readings can be off by 20-30% |
| Humidity | Below 80% relative humidity dry environment | Bathroom during showers open humid air | Premature chemical reactions; falsely high or low readings |
| Light Exposure | Dark drawer or cabinet opaque original vial | Windowsill or counter direct sunlight | UV damage to enzymes; strip degradation in days vs. months |
| Container | Original sealed vial cap closed tight always | Transfer to other containers vial left open | Loss of moisture barrier; all strips in vial compromised |
| Location Examples | Bedroom dresser drawer Climate-controlled room carry-on luggage | Bathroom medicine cabinet kitchen near sink checked luggage/car | Improper location combines multiple risk factors simultaneously |
Here’s what this means practically: storing your test strips in your bathroom (where humidity spikes during showers), in your car (where temperatures can soar), or near a sunny window can destroy their accuracy long before the expiration date. The ideal storage location is room temperature (68-77°F or 20-25°C) in a dark, dry place with the vial cap always tightly sealed.
The Risks of Using Expired Strips
You might be tempted to use those expired test strips “just this once” when you’ve run out, but consider this: using expired glucose test strips can lead to significantly inaccurate readings. For someone with diabetes making insulin dosing decisions, that kind of error isn’t just inaccurate—it’s potentially dangerous.
The enzymes in test strips break down over time, becoming less reactive to glucose. This means expired strips could show substantially higher or lower readings than your actual blood sugar level. Either scenario could lead to incorrect treatment decisions with serious consequences.
Lot-to-Lot Variability and Manufacturing Differences
Even when you’re using strips from the same manufacturer, research on lot-to-lot variability reveals that different production batches can show accuracy variations of up to 13%. This is why it’s crucial to code your meter correctly when you start a new vial of strips (for meters that require coding) and why you should run a control solution test with each new vial.
Some newer meters use “no-coding” technology that automatically adjusts for batch differences, but if you’re using an older meter, failing to update the code can introduce significant errors into your readings.
Contamination Risks and Hygiene Practices
Every time you touch a test strip, you transfer oils, moisture, and potentially other substances from your fingers to the strip. This is why you should always handle strips by their edges, never touching the test area. Additionally, if you’re testing in environments with food, lotions, or hand sanitizers present, even trace amounts on your fingertips can affect results.
One often-overlooked contamination risk: the vial itself. If moisture gets into your test strip container—even condensation from moving between temperature extremes—it can damage all the strips inside. This is another reason to keep the cap tightly closed except when removing a strip.
Proper Storage and Handling to Extend Test Strip Life
The good news is that with proper storage and handling techniques, you can ensure your test strips remain accurate for their full intended lifespan. Following these FDA-recommended best practices will help you get reliable results every time you test.
Best Practices for Storing Test Strips
First, always keep your test strips in their original container—never transfer them to another vial or storage container. The original vial is specifically designed with moisture barriers and often contains a desiccant to absorb any humidity that enters when you open it.
Second, establish a storage routine that minimizes exposure to damaging conditions:
- Store at room temperature (68-77°F) in a dark location away from direct sunlight
- Keep the vial in a drawer or cabinet, not on a bathroom counter or windowsill
- Close the cap immediately after removing a strip—don’t leave the vial open while testing
- Never refrigerate or freeze test strips unless specifically instructed by the manufacturer
- When traveling, keep test strips in your carry-on luggage at stable temperatures
- Write the date you opened the vial on the label so you know when to discard them
Avoiding Exposure to Environmental Extremes
Temperature fluctuations can be just as damaging as sustained heat or cold. If your test strips have been exposed to freezing temperatures (left in a car overnight in winter) or extreme heat (stored in a hot glove compartment), it’s safer to replace them rather than risk inaccurate readings.
The same applies to humidity exposure. If you live in a humid climate, consider storing your test strip vial in a cool, air-conditioned room rather than in a humid bathroom or kitchen. Some diabetes educators recommend keeping strips in a bedroom dresser drawer where temperature and humidity remain most stable.
Handling Tips to Prevent Contamination
Before testing, wash and thoroughly dry your hands with soap and warm water. If soap and water aren’t available, using an alcohol swab and allowing it to dry completely is acceptable—but handwashing is always preferred because it removes more potential contaminants.
Remove only one strip at a time from the vial, immediately recapping it. Hold the strip by its edges, insert it into your meter, and apply blood within the timeframe specified in your meter’s instructions (usually within a few seconds). Any delay between inserting the strip and applying blood can allow moisture from the air to affect the strip’s chemistry.
Continuous Glucose Monitors vs. Traditional Test Strips: Replacement Schedules
If you’re using or considering continuous glucose monitoring (CGM) technology, you need to understand that sensor replacement schedules are completely different from traditional test strips.
CGM Sensor Replacement Intervals
CGM systems use small sensors inserted under your skin that continuously measure glucose in your interstitial fluid (the fluid between cells) rather than testing blood directly. These sensors have predetermined wear times based on how long the enzyme coating remains active and accurate:
- Disposable CGM sensors: Typically last 7-14 days depending on the brand. Dexcom G6 and G7 sensors last 10 days, while FreeStyle Libre 2 sensors last 14 days.
- Implantable CGM sensors: The Eversense system uses a sensor implanted under the skin that lasts up to 180 days (6 months) before requiring replacement by a healthcare provider.
- Calibration requirements: Some CGM systems require periodic fingerstick tests with traditional test strips for calibration, while others (factory-calibrated systems) don’t require any fingerstick calibrations.
When to Consider CGM as an Alternative
While CGM technology offers real-time glucose monitoring and trend data that traditional test strips can’t provide, it doesn’t eliminate the need for test strips entirely. Most endocrinologists recommend having backup test strips available even if you use a CGM, because:
Sensor readings can be inaccurate during the first 24 hours after insertion, when glucose is changing rapidly, or if the sensor becomes dislodged. In these situations, confirming readings with a traditional fingerstick test ensures you’re making treatment decisions based on accurate data.
Signs Your Glucometer Test Strips Need Replacement
Beyond following replacement schedules, your test strips might be giving you warning signs that they’re no longer reliable. Recognizing these red flags can prevent you from making treatment decisions based on faulty data.
Inconsistent or Unexpected Readings
If you’re getting readings that don’t match how you feel, or if consecutive tests (using different strips) give you widely different results, your strips might be degraded. For example, if your meter shows 180 mg/dL but you have no symptoms of hyperglycemia, or if two tests taken one minute apart differ by more than 15%, it’s time to investigate.
First, run a control solution test to verify your meter is working correctly. If the meter passes but you’re still getting inconsistent readings, the test strips are likely the problem. Try a new vial from a different lot number—if readings stabilize, you’ve found your answer.
Physical Damage or Discoloration of Strips
Visually inspect your test strips before use. Strips should be uniform in color—any discoloration, darkening, or color changes indicate chemical degradation. Similarly, if strips appear bent, cracked, or damaged in any way, discard them immediately.
Also check the desiccant packet inside your vial. If it’s changed color (many desiccants turn from blue to pink when saturated with moisture), moisture has entered your vial and compromised your strips. In this case, replace the entire vial.
Meter Error Messages Related to Strips
Modern glucose meters are sophisticated enough to detect some problems with test strips. If your meter displays error messages like “strip error,” “check strip,” or “strip expired,” don’t ignore these warnings. These messages typically indicate that the meter detected an electrical or chemical problem with the strip.
While one error message might be a fluke (perhaps you inserted the strip incorrectly), repeated error messages with strips from the same vial suggest the entire batch is compromised.
Time-Based Replacement Guidelines
Even if your strips show no obvious problems, follow these time-based rules:
- Replace test strips 6 months after opening, even if the expiration date is later
- Never use strips past their printed expiration date, even if unopened
- If you test infrequently (once per week or less), consider buying smaller quantities that you’ll use within 3-4 months of opening
- When in doubt, run a control solution test—if results fall outside the acceptable range, replace your strips
Frequently Asked Questions
No, it’s not recommended. While the printed expiration date refers to unopened vials, once you break the seal and expose test strips to air, they begin degrading much faster. Most manufacturers specify that opened test strips should be discarded after 3-6 months, regardless of the expiration date. Using strips beyond this timeframe significantly increases your risk of inaccurate readings, potentially affecting your diabetes management decisions. If you test infrequently and find yourself discarding partially used vials, consider asking your healthcare provider about obtaining smaller quantities that you’ll use within the recommended timeframe.
Absolutely not—the FDA explicitly warns against purchasing used or pre-owned test strips. Here’s why this is dangerous: you have no way to verify how these strips were stored, whether they’ve been exposed to heat or humidity, if they’ve been tampered with, or even if they’re authentic. Pre-owned strips may have been removed from their original protective vial, stored in someone’s hot car, or be past their expiration date with the packaging altered. The money you might save isn’t worth risking inaccurate readings that could lead to hypoglycemia or hyperglycemia. Instead, explore legitimate cost-saving options like manufacturer discount programs, pharmacy savings cards, or discussing alternative strip brands with your doctor that might be more affordable while still being safe.
Test strips contain delicate enzymes (typically glucose oxidase or glucose dehydrogenase) that chemically react with the glucose in your blood. These enzymes are extremely sensitive to environmental conditions. High humidity causes moisture to penetrate the strip, which can trigger premature chemical reactions before you even apply blood, leading to falsely high or low readings. Heat accelerates enzyme degradation, essentially “aging” your strips faster than normal—strips exposed to 90°F temperatures might degrade in weeks rather than months. Cold temperatures can slow enzyme activity, potentially giving falsely low readings. According to research published in the Journal of Diabetes Science and Technology, test strip accuracy can decline significantly when exposed to temperatures above 86°F or humidity above 80% for just one week.
The printed expiration date on test strip packaging applies only to unopened vials stored under proper conditions. This date represents how long the manufacturer guarantees the strips will remain accurate when sealed in their original moisture-barrier packaging. However, once you open the vial and expose strips to air, a separate countdown begins. The “use by” date after opening is typically 3-6 months from when you first break the seal, and this date takes precedence over the printed expiration if it comes first. For example, if you open a vial with an expiration date of December 2025 in January 2025, you should discard those strips by July 2025 (6 months after opening), not December. Many manufacturers recommend writing the opened date on the vial label so you can track this accurately.
The FDA and most diabetes educators recommend running a control solution test in several situations: whenever you open a new vial of test strips, if you suspect your meter or strips aren’t working properly, if you’ve dropped your meter, if your test results don’t match how you feel, and at least once weekly if you test frequently. Control solutions contain a known amount of glucose, so when you test them, your meter should display a reading within the acceptable range printed on your test strip vial. If results fall outside this range, the problem could be either your meter or your test strips. This regular quality control is especially important if you rely on your glucose readings to make insulin dosing decisions, as it provides objective verification that your testing system is accurate.
Lot-to-lot variability refers to small manufacturing differences between batches of test strips, even from the same brand. Research published in the Journal of Diabetes Science and Technology found that test strips from different production lots can show accuracy variations of up to 13%. This happens because it’s nearly impossible to manufacture millions of test strips with absolutely identical enzyme concentrations and chemical compositions. This is why many meters require you to enter a code number from each new vial—this code tells the meter to adjust its calculations for that specific batch’s characteristics. Newer “no-coding” meters handle this automatically. To minimize the impact of lot-to-lot variability, run a control solution test whenever you start a new vial, and if you notice your readings seem different with a new vial, verify the change is real (not just variability) by testing at consistent times and comparing patterns rather than individual readings.
Yes, even CGM users should maintain a supply of current, properly stored test strips as backup. CGM sensors have different replacement schedules (typically 7-14 days for disposable sensors), but they’re not infallible. You’ll need traditional test strips in several situations: during the first 24 hours after inserting a new sensor when readings may be less accurate, when you’re experiencing symptoms that don’t match your CGM reading, if your CGM shows rapid glucose changes (when interstitial fluid readings lag behind blood glucose), if your sensor fails or falls off unexpectedly, or for calibration if you use a CGM system that requires fingerstick verification. Most endocrinologists recommend CGM users keep at least one current vial of test strips (replaced every 6 months) available for these situations. Additionally, some diabetes management situations—like adjusting insulin during illness—may require more frequent verification testing than CGM alone provides.
Taking Control of Your Glucose Monitoring Accuracy
Understanding when and why to replace your glucometer test strips isn’t just about following rules—it’s about ensuring that every treatment decision you make is based on accurate, reliable data. The test strips you use are sophisticated medical devices that require proper storage, handling, and timely replacement to work correctly.
Test Strip Management Checklist
- Use each strip only once — Never reuse or buy pre-owned strips
- Write opened date on vial — Discard after 3-6 months regardless of expiration
- Store at room temperature — 68-77°F in dark, dry drawer (not bathroom)
- Keep vial tightly closed — Original container only, cap sealed immediately after use
- Check expiration dates — Never use expired strips, even if unopened
- Run control solution tests — Every new vial, weekly if testing frequently, when suspicious
- Inspect before using — Discard if discolored, bent, or desiccant packet changed color
- Handle by edges only — Wash hands before testing, don’t touch test area
- Protect from extremes — No car storage, direct sunlight, or humidity exposure
- Keep backup supply (CGM users) — Fresh vial for sensor failures or confirmation testing
Remember these critical takeaways: always use single-use test strips only once, replace opened vials within 3-6 months regardless of expiration dates, store strips in their original container in cool, dry conditions away from environmental extremes, never use expired strips or buy pre-owned strips, and run control solution tests regularly to verify accuracy. Whether you’re using traditional test strips multiple times daily or maintaining a backup supply alongside your CGM system, these practices ensure you’re making informed decisions about your diabetes management.
The small investment of replacing test strips on schedule and storing them properly pays enormous dividends in accurate readings and confident diabetes control. Talk with your healthcare provider about the most cost-effective testing strategy for your situation, including assistance programs that might be available. Your glucose readings guide everything from meal planning to insulin dosing—make sure those readings are trustworthy by following the evidence-based guidelines outlined in this article.
What’s your biggest challenge with managing test strip replacement and storage? Share your questions with your diabetes care team at your next appointment to develop a system that works for your lifestyle and testing frequency.
References and Sources
- U.S. Food and Drug Administration. (2021). “How to Safely Use Glucose Meters and Test Strips for Diabetes.” FDA Consumer Update. Available at: https://www.fda.gov/consumers/consumer-updates/how-safely-use-glucose-meters-and-test-strips-diabetes
- Klonoff, D. C. (2010). “Self-Monitoring of Blood Glucose: Practical Aspects.” Journal of Diabetes Science and Technology, 4(2), 435-439. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC2864180/
- Baumstark, A., et al. (2012). “Lot-to-Lot Variability of Test Strips and Accuracy Assessment Criteria.” Journal of Diabetes Science and Technology, 6(5), 1076-1086. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC3570841/
- National Institute of Diabetes and Digestive and Kidney Diseases. (2024). “Continuous Glucose Monitoring.” NIDDK Health Information. Available at: https://www.niddk.nih.gov/health-information/diabetes/overview/managing-diabetes/continuous-glucose-monitoring
- Ginsberg, B. H. (2009). “Factors Affecting Blood Glucose Monitoring: Sources of Errors in Measurement.” Journal of Diabetes Science and Technology, 3(4), 903-913. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC5032951/
- American Diabetes Association. (2024). “Standards of Medical Care in Diabetes.” Diabetes Care, 47(Supplement 1). Available at: https://www.diabetes.org/
- Centers for Disease Control and Prevention. (2024). “Diabetes: Managing Your Blood Glucose.” CDC Diabetes Prevention and Control. Available at: https://www.cdc.gov/diabetes/
Disclaimer:
The information provided on MD-Pilot is for educational and informational purposes only. It is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified healthcare provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.
Recomended Articles
View AllWeekly Health Intel
Get evidence-based health tips, latest research, and exclusive guides delivered weekly